Modern dentistry has advanced far beyond traditional X-rays, allowing dentists to diagnose oral health issues with greater precision than ever before. One of the most significant innovations in dental imaging is Cone Beam Computed Tomography (CBCT), a technology that provides detailed three-dimensional images of the teeth, jaw, nerves, and surrounding structures.
While many dental problems can be identified through routine examinations and standard X-rays, some conditions remain hidden beneath the surface. CBCT imaging helps uncover these issues early, leading to more accurate diagnoses, effective treatment planning, and better patient outcomes.
What Is CBCT Imaging?
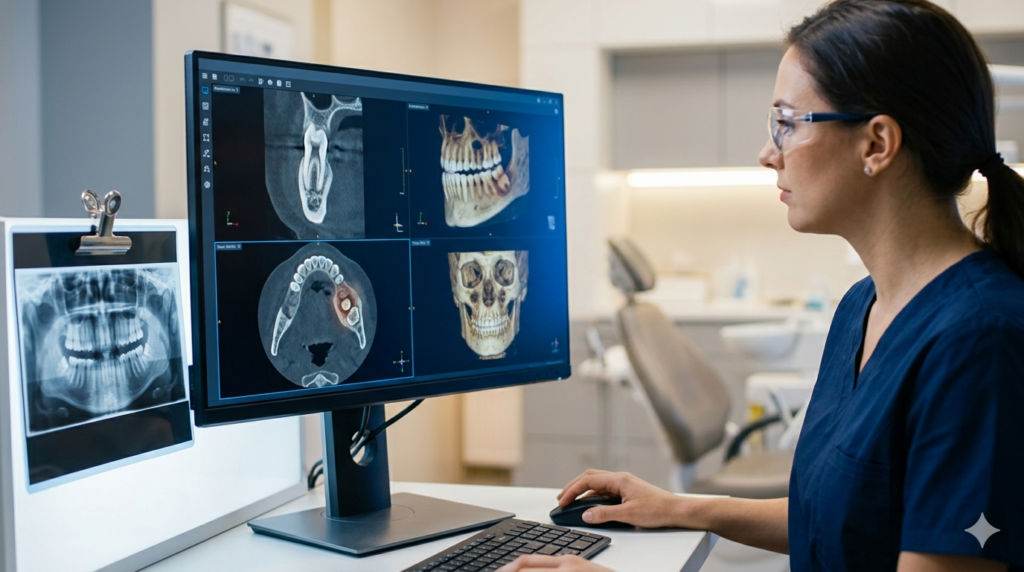
CBCT (Cone Beam Computed Tomography) is a specialized imaging technology that captures hundreds of images from different angles and combines them into a detailed 3D view of the mouth and facial structures.
Unlike traditional dental X-rays, which provide only two-dimensional images, CBCT scans allow dentists to examine oral structures from multiple perspectives. This enhanced visibility makes it easier to detect conditions that may otherwise go unnoticed.
The scanning process is quick, comfortable, and non-invasive, typically taking less than a minute to complete.
Why Traditional X-Rays May Not Show Everything
Standard dental X-rays remain an important diagnostic tool, but they have limitations. Since they produce flat, two-dimensional images, certain structures can overlap, making it difficult to identify hidden problems accurately.
In some cases, conditions such as infections, bone loss, impacted teeth, root fractures, or abnormalities within the jaw may not be fully visible on conventional X-rays.
CBCT imaging provides a comprehensive view that eliminates much of the guesswork, helping dentists make more informed clinical decisions.
Hidden Dental Problems CBCT Can Detect
- Impacted Teeth
Wisdom teeth and other impacted teeth can develop beneath the gums without causing obvious symptoms initially. CBCT scans reveal their exact position and relationship to nearby teeth, nerves, and bone structures.
This information is especially valuable when planning safe and effective tooth extractions.
- Root Fractures and Cracks
Tiny cracks in tooth roots can be difficult to detect using traditional imaging methods. These fractures often cause unexplained pain, sensitivity, or recurring infections.
CBCT imaging provides detailed views of the tooth structure, helping dentists identify fractures that may otherwise remain hidden.
- Bone Loss and Periodontal Disease
Gum disease can lead to significant bone loss around teeth. CBCT scans offer a precise evaluation of bone levels, enabling dentists to assess the severity of periodontal disease and create targeted treatment plans.
Early detection of bone deterioration can help preserve natural teeth and prevent future complications.
- Dental Infections and Abscesses
Some infections develop deep within the jawbone or around tooth roots and may not be easily visible during a routine examination.
CBCT imaging can locate hidden infections, abscesses, and areas of inflammation, allowing dentists to address the problem before it spreads or causes extensive damage.
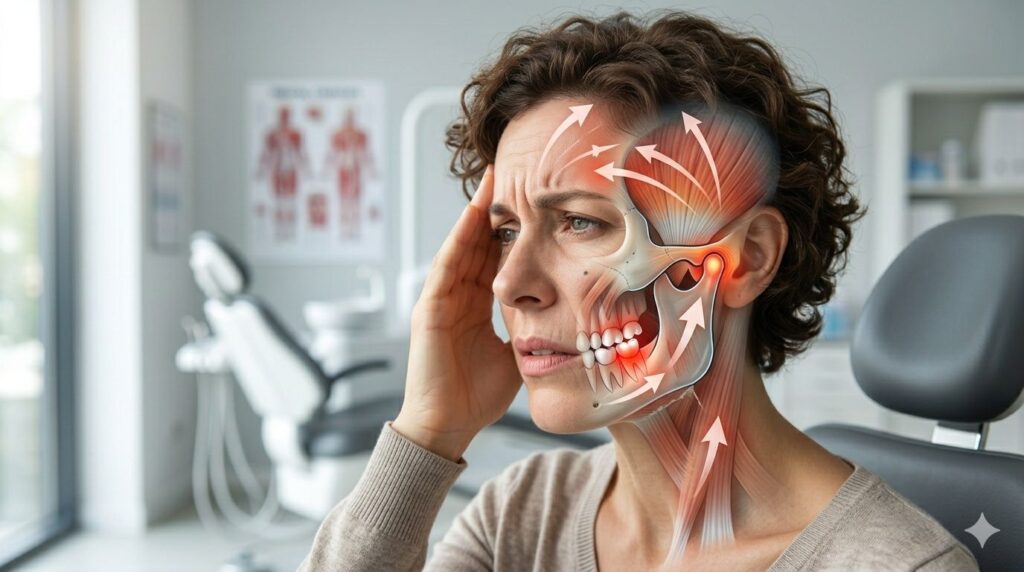
- Jaw Joint (TMJ) Disorders
Patients experiencing jaw pain, clicking sounds, headaches, or difficulty chewing may have temporomandibular joint (TMJ) disorders.
CBCT scans provide detailed images of the jaw joints, helping dentists evaluate structural abnormalities and determine the most appropriate treatment approach.
- Cysts, Tumors, and Other Abnormalities
Although uncommon, cysts, tumors, and other growths can develop within the jaw and surrounding tissues. CBCT imaging allows for early detection of these abnormalities, increasing the likelihood of successful treatment.
Benefits of CBCT Imaging for Patients
More Accurate Diagnoses
The detailed 3D images produced by CBCT technology allow dentists to identify issues with greater confidence and precision.
Improved Treatment Planning
Whether you’re receiving dental implants, root canal therapy, orthodontic treatment, or oral surgery, CBCT scans provide essential information that helps ensure safer and more predictable results.
Early Detection
Many dental conditions become more complex and costly to treat when left undiagnosed. CBCT imaging helps identify problems at an earlier stage, allowing for prompt intervention.
Better Patient Understanding
The three-dimensional images make it easier for patients to visualize their oral health conditions and understand recommended treatment options.
When Might Your Dentist Recommend a CBCT Scan?
Your dentist may suggest CBCT imaging if you:
- Need dental implants
- Have impacted wisdom teeth
- Experience unexplained tooth pain
- Require root canal treatment
- Show signs of advanced gum disease
- Have jaw joint concerns
- Need oral surgery or complex treatment planning
Not every dental visit requires a CBCT scan, but it can be an invaluable diagnostic tool when detailed information is needed.
CBCT imaging has revolutionized modern dentistry by providing a clearer, more comprehensive view of oral structures than traditional X-rays alone. Its ability to detect hidden dental problems helps dentists diagnose conditions earlier, plan treatments more accurately, and improve overall patient care.
If you’re experiencing unexplained dental symptoms or are preparing for a specialized dental procedure, CBCT imaging may provide the insights needed to protect your oral health and ensure the best possible treatment outcome.